- Home
- Medical Thermography Research
Medical Thermography Research

Advanced Thermography
Early Detection, Backed by Research
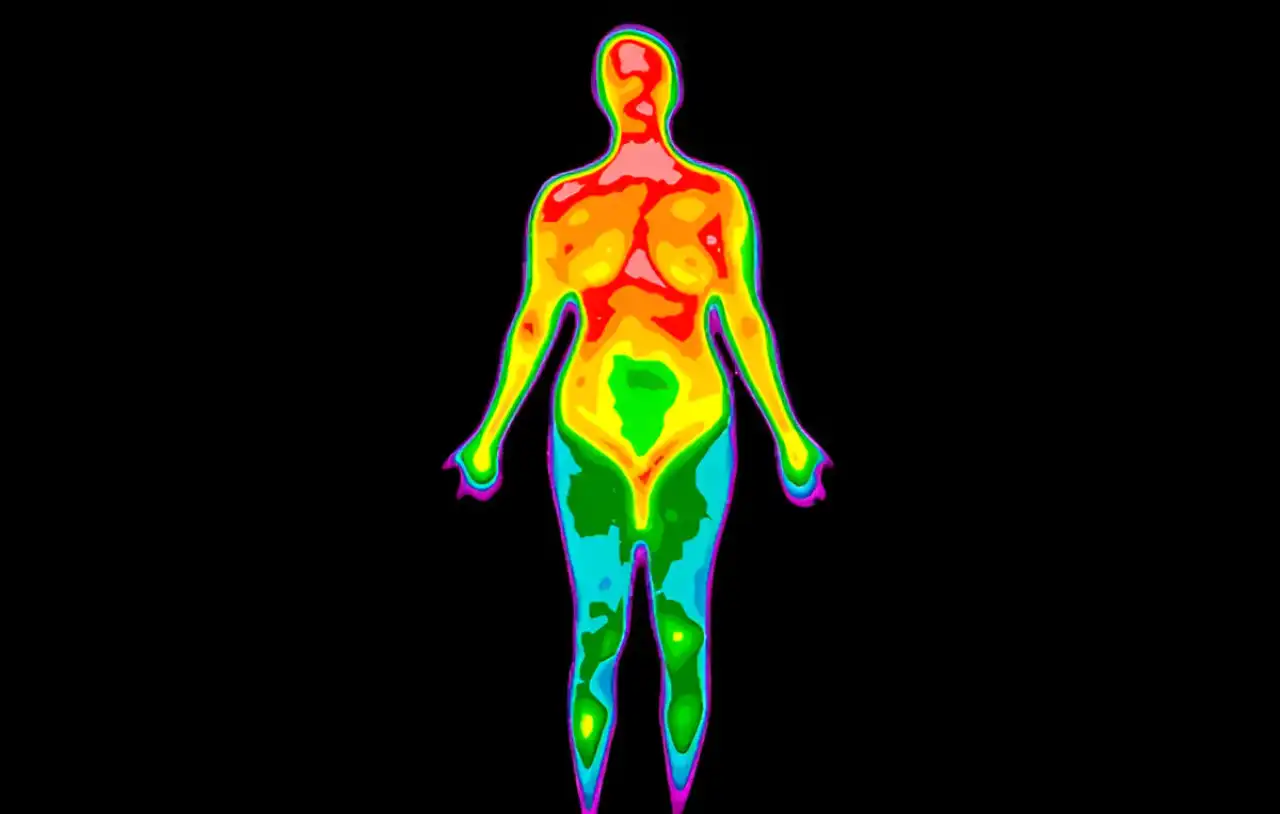
Medical thermography research has shown that thermography is a cutting-edge, non-invasive imaging technique that detects abnormal heat patterns in the body. It is especially valuable for monitoring breast health and aiding in cancer detection. Unlike traditional methods like mammography, thermography can identify changes at an earlier stage. Extensive medical thermography research, including over 800 peer-reviewed studies involving 250,000 women, highlights its effectiveness in early disease detection. As technology advances, thermography continues to gain recognition as a vital tool in preventive healthcare.
The Cornell Study, 2008 – How Thermography Detects Breast Cancer
Studies show that thermography is highly effective in detecting breast cancer. In fact, the Cornell Study found that thermography had a 97% success rate in spotting malignancies. Researchers examined how thermography detects abnormal heat patterns linked to cancer. As a result, they concluded that thermography improves early detection, especially when combined with other screening methods. Therefore, adding thermography to standard screenings can help save lives.
Thermography’s Role in Breast Health
As breast cancer cases rise globally, thermography has become a vital tool for monitoring health. This study highlights how thermography identifies early warning signs in breast tissue. Because of its ability to detect subtle temperature changes, thermography helps assess risks before physical symptoms appear. Furthermore, it offers a safe, radiation-free option for ongoing screening, which makes it ideal for younger women.
Explore the PACT Journal for Thermography Research
Stay informed on the latest research in thermography and its role in detecting diseases early. The PACT Journal offers peer-reviewed studies and in-depth analysis of thermography’s impact on healthcare. By reading the journal, you can learn how thermography is shaping the future of medical imaging.